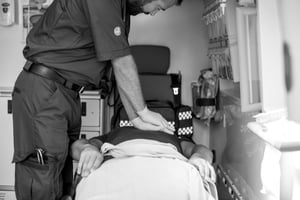
 Resuscitation is required whenever a patient is unable to breath or their heart stops beating. This may be due to a medical condition such as a heart attack or a result of trauma caused by an accident. While cardiopulmonary resuscitation (CPR) is essential, hypothermia may occur, especially in instances of trauma, and exacerbate the patient's condition, leading to long term complications and even death. EMS personnel need to be cognizant of this risk, and if there's any indication of hypothermia, take immediate steps to warm the patient.
Resuscitation is required whenever a patient is unable to breath or their heart stops beating. This may be due to a medical condition such as a heart attack or a result of trauma caused by an accident. While cardiopulmonary resuscitation (CPR) is essential, hypothermia may occur, especially in instances of trauma, and exacerbate the patient's condition, leading to long term complications and even death. EMS personnel need to be cognizant of this risk, and if there's any indication of hypothermia, take immediate steps to warm the patient.
Why the Risk of Hypothermia?
Hypothermia occurs when a person's core body temperature drops below 95 °F (35 °C). This happens when the body can't generate enough warmth to counter heat lost to the environment. Initially, the body tries to counter this by shivering. If this doesn't work, the core temperature continues to fall and organs such as the brain and heart slow down, leading to difficulty in breathing. This causes oxygen deprivation and mental confusion, resulting in an inability to make rational decisions.
Factors That Contribute Toward Hypothermia
While exposure to cold increases the risk of hypothermia, it can be caused by other factors as well. These include illnesses such as diabetes, heart disease, exhaustion, alcohol and medication. Homeless and poor people without adequate heating are susceptible, as are children, especially if they are inadequately dressed for the weather. Hypothermia as a result of trauma arising from vehicular and other accidents is another factor, particularly if patients are seriously injured and bleeding.
Identifying Patients Suffering from Hypothermia
While the clinical definition of hypothermia is anyone whose core body temperature is below 95 °F, in practice it's not easy to determine this when in the field. Instead the best way is to check for physical symptoms such as:
- Shallow breathing
- Weak pulse
- Shivering
- Dizziness
- Slurred speech
- Poor coordination
- Confusion
- Memory loss
- Drowsiness
- Pale skin coloration
If a patient is suffering from severe hypothermia they may:
- Lose consciousness
- Stop shivering
- Have no pulse
- Develop low blood pressure
If there's any doubt, it's best to assume that a patient is suffering from hypothermia.
Dealing with Hypothermia
If the patient is unconscious, apply CPR. Once they're breathing, move them to a warm, dry location. When placing them in the ambulance, make certain it's been warmed to well above ambient temperature. Remove all wet or damp clothing and cover the patient with a warm blanket. If it's not immediately possible to move the patient, insulate them as much as possible. Avoid removing clothing unnecessarily, but if this has been done as part of patient evaluation and treatment, make sure they are adequately covered.
If the patient is conscious and able to respond, provide them with a warm nonalcoholic drink. As soon as possible, measure the patient's temperature and monitor its trend. If there's a need for an IV, always use fluids that have been warmed to above room temperature to avoid reducing the patient's core temperature further. Keep them warm with a thermal, cotton or fleece blanket.
When resuscitating patients with hypothermia, it's important to keep them warm and to monitor their temperature constantly. For this reason, it's advisable to use the most appropriate blankets for the ambient conditions. Use this guide to selecting the right medical blanket. To find out more, contact us at Graham Medical.

